Since 25 August, MSF has massively scaled up its operations in Cox’s Bazar, Bangladesh.
Number of MSF health facilities: 19 health posts, three primary health centres and four inpatient health facilities
Number of staff: 2,258 national and international staff as of the end of November
Number of patients: 142,985 patients have been treated at MSF outpatient facilities and 3,117 patients in inpatient facilities between the end of August and the end of November
Main morbidities: respiratory infections, diarrhoeal diseases, measles, and an increase in diphtheria cases
Other activities: water and sanitation (water trucking, hand pump, tube well and latrine installation) and mental health services
We now manage 19 health posts, three primary health centres and four inpatient facilities. Around 2,300 people work for MSF in the Cox’s Bazar district. The main morbidities among patients in our clinics are respiratory tract infections, diarrhoeal diseases and increasing cases of infant malnutrition, which are directly related to the poor living conditions, particularly the state of shelter, water and sanitation in the settlements.
By the end of November, we saw 2,165 cases of measles across all MSF health facilities and more than 77 cases of jaundice.
In addition, the number of suspected diphtheria cases we see at our health facilities has increased. By 21 December, we had treated more than 2,000 patients, most of whom were aged between five and 14 years.
Without an antitoxin, diphtheria can result in a high case-fatality rate. Only a limited quantity arrived in Bangladesh recently.
Active case investigation began in most of the settlements where MSF is working to see if anyone else was sick in the patients’ households. We also collected information about the number of household members and any other contacts the patients had prior to presentation. Contacts are being treated prophylactically with antibiotics via the health facilities. The preparation and establishment of a reserved isolation area for suspected cases are ongoing.
Most of these vaccine-preventable diseases are further examples of how little access the Rohingya population in Myanmar had to routine healthcare. We’ve worked on expanding our isolation capacity for measles and other infectious diseases in most of our facilities.
In response to inpatient capacity needs, we’ve increased the number of beds at our facilities in Kutupalong and our newly-built health facility in Balukhali. We’ve also opened a new 25-bed inpatient facility in the Tasnimarkhola settlement. It’s the only inpatient centre in the area. Another, which was due to open near Moynarghona makeshift settlement, is functioning as a temporary 85-bed diphtheria treatment centre.
In preparation for a potential outbreak of cholera or other diarrhoeal diseases, we have identified sites for diarrhoea treatment units in Balukhali, Hakimpara, Jamtoli, and Unchiprang. Preparations are ongoing.
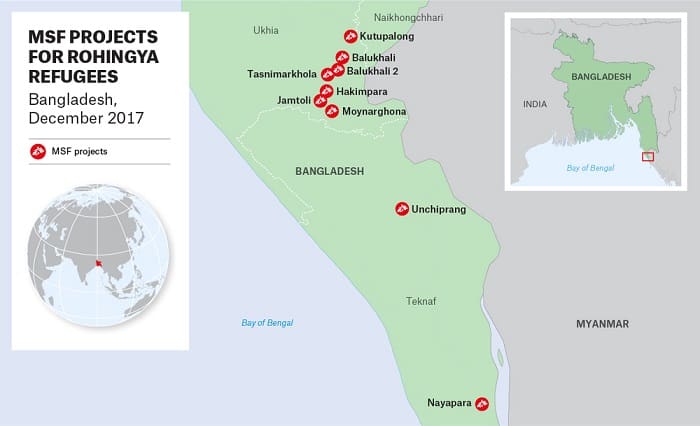
MSF project locations in Cox’s Bazar
Kutupalong
More than 547,000 refugees are now living in makeshift settlements in Kutupalong and Balukhali, as well as the expansion site. The MSF Kutupalong health facility has operated since 2009 and is our biggest in Cox’s Bazar. Among the services in this clinic are: a 24-hour emergency room; an outpatient department; an inpatient department, which includes a paediatric and neonatal ward; isolation beds; a diarrhoea treatment ward; sexual and reproductive healthcare services; a mental health department, and basic laboratory services.
Since 25 August, the inpatient department has expanded from 50 to 79 beds to cope with the influx and the increasing numbers of patients. Its isolation capacity was also increased to cope with a potential outbreak of communicable diseases. The outpatient department treats more than 300 patients per day. We plan to rehabilitate the hospital, increase the number of beds and improve the overall infrastructure in the hospital to meet the needs of the growing population. Construction work began in November and will continue through to the new year.
MSF has built and manages three health posts in Kutupalong makeshift settlement expansion area. The health posts treat over 300 patients per day and are located throughout the settlement to provide access to newly arrived refugees.
Balukhali
At the end of October, we opened a 40-bed mother and child inpatient facility in Balukhali, near the existing outpatient clinic. In early December, this was converted into a diphtheria treatment centre in response to the rapidly growing outbreak of the disease. We now have 70 beds in the facility for treating diphtheria patients. We also run three health posts in this settlement.
Balukhali 2
Since 1 October, MSF has run a health post in Balukhali 2, which has a population of 285, 000. The health provides basic primary healthcare and treated more than 18,100 people between 1 October and 11 December. Newly arrived refugees are being settled in the zone named SS, which includes Balukhali 1 and Balukali 2. On 18 November, MSF opened a health post in the SS zone that treats an average of 170 patients per day.
Tasnimarkhola
More than 58,000 refugees live in Tasnimarkhola’s makeshift settlement, formerly known as Burma Para. MSF opened a health post on 26 October and treated 12,400 patients by 11 December. Around 30 percent of consultations, here are for children under five. On 3 December, we started sexual and reproductive health activities (antenatal, postnatal, sexual and gender-based violence, gynaecological consultations and family planning).
On 26 November, we opened a 25-bed inpatient facility. The hospital focuses on paediatrics (children below the age of 15), inpatient treatment of severe acute malnutrition (10 percent of hospitalised patients) and the management of measles cases (55 percent of hospitalised patients). To accommodate the high number of measles cases, we had to increase the number of isolation beds to 36. By 11 December we received 320 patients in the emergency room. Of these, 171 (53 percent) were hospitalised.
We’ve drilled four deep production boreholes to provide water to the health posts and inpatient department.
Unchiprang
More than 23,300 refugees live in Unchiprang’s makeshift settlement. MSF runs a primary health centre, which initially opened as health post in mid-September. We provide around-the-clock primary healthcare, sexual and reproductive healthcare and mental health services, with 10 hospitalisation beds. We are the main health-care provider in the settlement and our team carries out more than 150 consultations per day. We’ve opened a second health post in Uchiprang and another in nearby Nayapara and treat 200 cases daily in both.
Jamtoli
Jamtoli makeshift settlement has a population of 48,400. The health post MSF opened there in September was later upgraded later to a primary healthcare centre. The clinic currently receives up to 250 patients per day and offers 24-hour primary health care service, with a delivery room and 18 hospitalisation beds. We run two other health posts in Jamtoli.
Hakimpara
More than 33,000 refugees live in Hakimpara’s makeshift settlement. The health post we opened there has been upgraded to a primary healthcare centre with 24-hour primary health care services and 14 hospitalisation beds. We treat around 150 patients per day there. We also run two other health posts.
Moynarghona
More than 19,500 refugees live in Moynarghona’s makeshift settlement. MSF started a mobile clinic in September, which has since been upgraded to a health post. The clinic sees an average of 200 patients per day. Before the end of the year, we plan to open an inpatient department with a 63- bed capacity outside the settlement. It will offer an emergency room and a paediatric and inpatient therapeutic feeding centre for the Rohingya and host communities. In the meantime, this site has been used as an 85-bed diphtheria treatment centre since 11 December.
Sabrang entry point
On 8 October, we started a mobile clinic at the border point in Sabrang, offering nutritional screening and basic healthcare and monitoring. Its services have been integrated into the reception centre’s circuit.
Other activities
Vaccination
MSF is vaccinating children and pregnant women in its facilities to support the government’s initiative to expand routine vaccination in the camps. Staff at all our health facilities will have the capacity to administer immunisation for measles and rubella, oral polio and tetanus according to national protocols.
From 18 November, the Ministry of Health ran a 12-day measles and rubella vaccination catch-up campaign targeting more than 336,000 children between the age of six months and 15 years. MSF supported this campaign with community mobilisation, site identification, logistics and the transportation of vaccines. A vaccination coverage survey is planned in mid-December to evaluate the success of the campaign.
Sexual violence
Key figures:
- Total number of sexual violence cases from 25 August to 3 December: 113
- Number of rape cases: 91
- Number of sexual and gender-based violence cases under the age of 18: 37
- Number of cases of male on male sexual violence: 0
Since 25 August, we’ve treated 113 survivors of sexual violence at our sexual and reproductive health unit in Kutupalong. Of these, 33 percent were under the age of 18, including one under the age of ten.
Estimating the number of survivors is not possible. But sexual violence is often under-reported due to stigma and shame, fear of reprisals, a lack of knowledge about the medical consequences of sexual violence and the need for timely medical care, and a lack of awareness about the medical and psychological support available.
Given these barriers, it is likely that the number of survivors of sexual and gender-based violence MSF has treated so far is just a fraction of reality.
We are starting to see more survivors seeking medical care because some of these women and girls have become pregnant as a result of rape.
MSF has specialised staff on the ground to treat survivors who are referred for treatment as a result of trauma, including sexual assault and rape. Our local community outreach workers visit people living in the settlements and inform them about our free services, which include treatment for sexual violence.
Water and Sanitation (WASH)
Beyond our medical response, improving water and sanitation is a major part of our attempts to prevent the spread of disease. According to the WHO[1], 91 per cent of households and 60 percent of source samples were contaminated with Escherichia coli (E. coli). Due to the lack of a drainage system, stagnant water is present in 26 percent of all tube wells. As for sanitation, 39 percent of emergency latrines installed by WASH partners, mostly at the early stage of the emergency response, are non-functional. The desludging and decommissioning of these latrines remains a priority to improve the inadequate sanitation environment.
MSF is targeting its water and sanitation response in the most difficult to reach areas. So far, we have built 1,247 latrines, 157 water wells and a gravity water supply system in the settlements located in the north and south.
By the end of December, we aim to install 400 boreholes and 1,000 latrines in the Balukhali and Kutupalong makeshift settlements. As the shallow aquifer (the main water source, abundant in quantity and easy to access) is contaminated with fecal coliforms throughout the camps, we started drilling production boreholes between 150 and 200 metres deep to have clean water. To date, four deep boreholes have been drilled.
We plan to start hygiene promotion, clean latrines, educate about hand washing, and distribute soap and other non-food items in MSF facilities. To ensure vulnerable population have clean drinking water, we also plan to distribute water filters in our clinics in Tasnimarkhola and Balukali 2 to patients with malnutrition and measles, and pregnant women. In the southern settlements of Unchiprang and Jamtoli, we aim to build 56 more latrines and 43 wells in the coming weeks.
Our emergency response for new arrivals also includes water supply and sanitation. We have deployed teams to arrival, transit and settlement locations to ensure that newly arrived refugees have access to safe drinking water and adequate sanitation facilities.
As the settlements continue to expand, refugees have inequitable access to basic needs such as healthcare services, food and water. The military is currently working on a new road but additional improvements and humanitarian services are urgently needed to ensure aid is reaching all those with basic needs and to limit further hardship and the risk of public health problems.
[1] Morbidity and Mortality Weekly Bulletin Vol. 8, 3 December 2017: https://www.searo.who.int/bangladesh/mmwb/en/











