Iraq has long suffered from war and political instability. The most recent conflict ended in 2017, when Mosul was recaptured after almost three years under the control of the Islamic State (IS) group.
Three years later, the consequences of the conflicts in Mosul are still evident. One is the terrible impact on medical care, as many health facilities in Mosul were completely destroyed.. The city’s inhabitants are left with a fragile health system that barely meets their most basic needs. Mosul is located in Ninewa governorate, home to a population of 3.5 million, with only one hospital bed for every 3,000 people.
When COVID-19 reached Mosul earlier this year, it was clear that the local health system would struggle to control the outbreak. Countrywide measures adopted by the Iraqi government initially succeeded in slowing its spread but, in the past two months, cases have risen steeply. In Mosul, in early August, there were 30 times more COVID-19 patients than in previous months, while cases across the country rose from 10,000 to more than 120,000.
Soon after the pandemic was declared, MSF took the decision to support Mosul’s healthcare system’s handling of the outbreak, temporarily transforming its 62-bed post-operative care centre in the east of the city into a COVID-19 treatment facility for suspected and confirmed cases.
MSF head nurse Ali Alzubaidi has worked in the medical facility for years caring for patients in need of extensive surgery but he now looks after people with COVID-19 symptoms.
“With the emergence of the virus, we had to change our activities,” says Ali. “All the staff were trained in infection prevention and control. We adapted our treatment protocols and prepared the facility for isolating and treating COVID-19 patients. So far, we have received more than 769 cases including 312 confirmed patients.”

On the far side of the river, in west Mosul, which bore the brunt of the destruction during the battle for the city, MSF runs a hospital providing a range of essential services, including emergency treatment and stabilisation, emergency obstetric and neonatal care, inpatient pediatric care, and mental healthcare.
“For us, keeping such services running, even in times of COVID-19, was unquestionable,” says Dr Humam Nouri. “This is one of the few functioning hospitals in this part of the city, and the pandemic doesn’t erase all the population’s health needs.”
The hospital is as busy as ever, says Dr Humam, who has worked in the emergency room for the past 18 months.
“The number of patients we see on a daily basis has not decreased since the beginning of the pandemic,” he says. “We still see about 100 people a day, suffering from all sorts of injuries. And in the maternity ward, many women are still coming to give birth.”
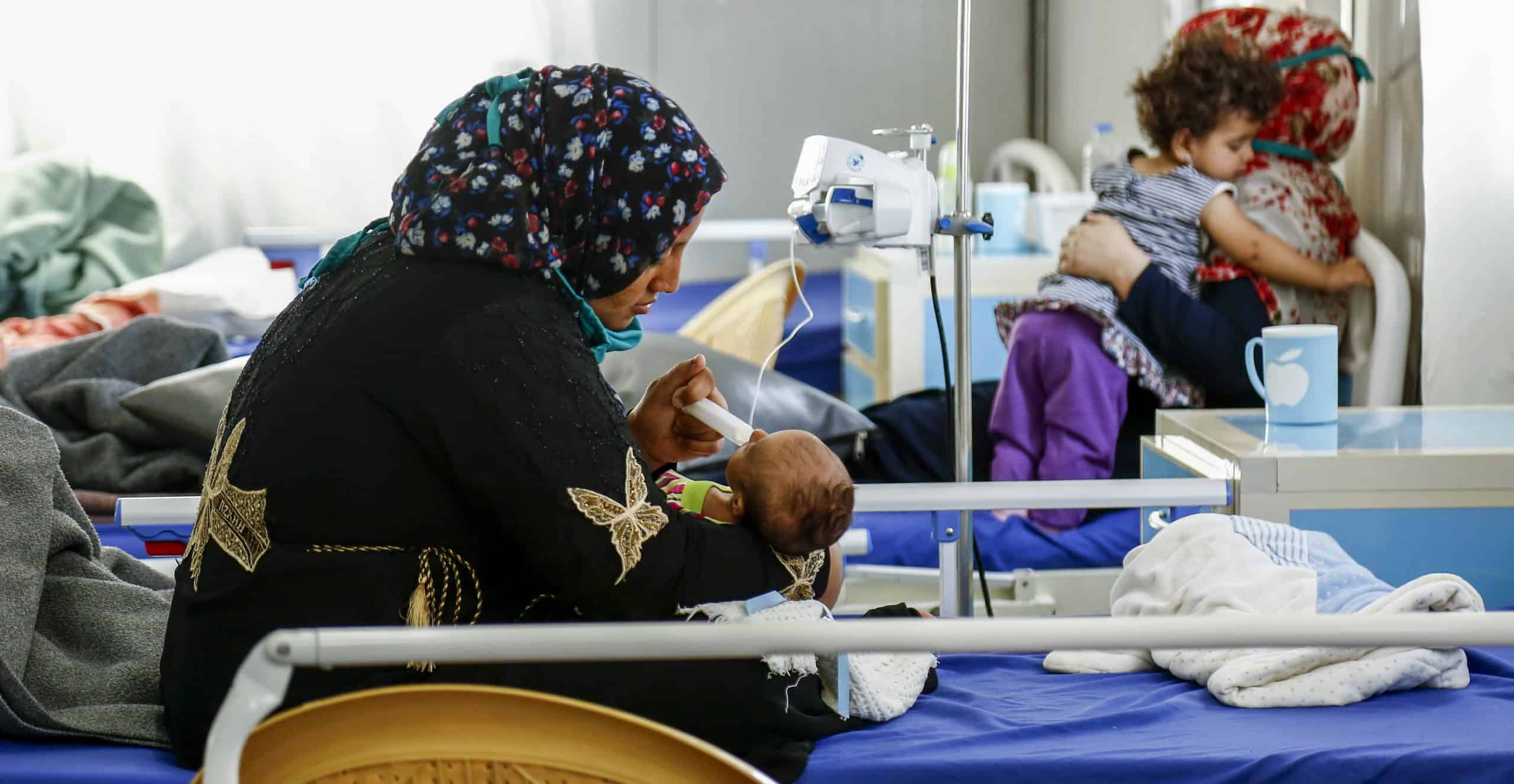
On both sides of the city – in MSF’s COVID-19 centre in east Mosul and in its hospital in west Mosul – the virus has brought additional challenges. For patients, it is harder to reach hospital since movement restrictions were imposed as part of a wider lockdown to contain the spread of the virus.
During curfew hours, the only people to arrive are those suffering medical emergencies, while people who live beyond the city limits have to negotiate multiple checkpoints to reach medical care, with the result that some only arrive when it is too late.
“I feel heartbroken when a patient arrives too late at the emergency room,” says Dr Humam. “I think these deaths are a side effect of the pandemic that people tend to underestimate.”
The stigma associated with COVID-19 is another major issue and has a direct impact on people’s use of essential health services.
“Our health promotion teams have talked to dozens of patients. They find that misinformation and social stigma regarding COVID-19 causes reluctance to seek healthcare for patients experiencing COVID-19 symptoms,” says Itta Helland-Hansen, MSF’s field coordinator in the COVID-19 treatment centre in east Mosul.
“We need to challenge misconceptions and to insist on the fact that the earlier COVID-19 symptoms are addressed, the better it is for the patients themselves and for the community at large.”
“Our teams dedicate time to sharing information with patients about how the disease spreads and how to stay safe,” says Ali Alzubaidi. “But we can expect the numbers of COVID-19 patients to carry on rising if people continue to forgo protective measures and delay seeing a doctor when they get sick.”
To tackle the issue of misinformation, MSF recently started an online campaign in Mosul to raise awareness about health precautions that people can take to protect themselves against COVID-19.

Elsewhere in Iraq, MSF is also working to help the health system cope with the pandemic. In the capital Baghdad – the city hardest hit by the virus – MSF is supporting two COVID-19 treatment centres (Ibn Al-Khateeb and Al-kindi) and providing training on patient triage and infection prevention and control, and on-the-job coaching to staff in Al-Kindi intensive care unit.
MSF teams have been providing training sessions, with a focus on infection prevention control, at health facilities in Erbil, Dohuk and Ninewa governorates. MSF has also set up a 20-bed isolation and treatment facility in Laylan camp in preparation for a potential spike of COVID-19 cases there. MSF has kept its regular medical services running in Kirkuk governorate, where it provides much needed healthcare for mothers and patients with non-communicable diseases.
“What we’re doing in Mosul is just one example of what we’re trying to do on a larger scale across the country,” says Marc van der Mullen, MSF head of mission in Iraq. “In a country like Iraq, maintaining our existing services and responding to emergencies are equally important right now. We have no choice but to adapt our operations and try to work on both fronts.”
-
Related:
- coronavirus
- COVID-19
- Iraq
- Mosul
- War











