By Aparna Iyer, Project Medical Referent, MSF Drug-Resistant Tuberculosis Project in Mumbai
MSF’s drug-resistant tuberculosis (DR-TB) and HIV project is located in the M-East Ward, one of the TB high-burden areas in Mumbai. During the second wave, there was a high number of COVID-19 cases being reported, about 6,000-7,000 cases a day which forced authorities to impose a complete lockdown in the state. This week, the number of new cases of COVID-19 have reduced in Mumbai as we are seeing around 3,000 cases everyday.
It is important that services are interrupted for TB patients who have complex resistant patterns. In MSF’s independent clinic and the OPD run in collaboration with the National TB elimination programme, we’ve adapted to restrictions and for the last three weeks, we are physically present in the clinic on alternate days to see new patients and provide consultations to severely ill. We’re still diagnosing a lot of new patients with TB who were unable to seek help due to the movement restrictions.
On the other days, the medical team works from home carrying out virtual medical consultations and psychosocial support to our patients by phone. If necessary, they can be prescribed medication on WhatsApp that can be collected from local pharmacies. Otherwise, patients can be referred to nearby hospitals for any side effect management or labs for any investigation if needed
The community health workers who used to do home visits for contact tracing and educate the community about TB are now also following up with the patients and providing support over the phone to keep the community and our health workers safe.
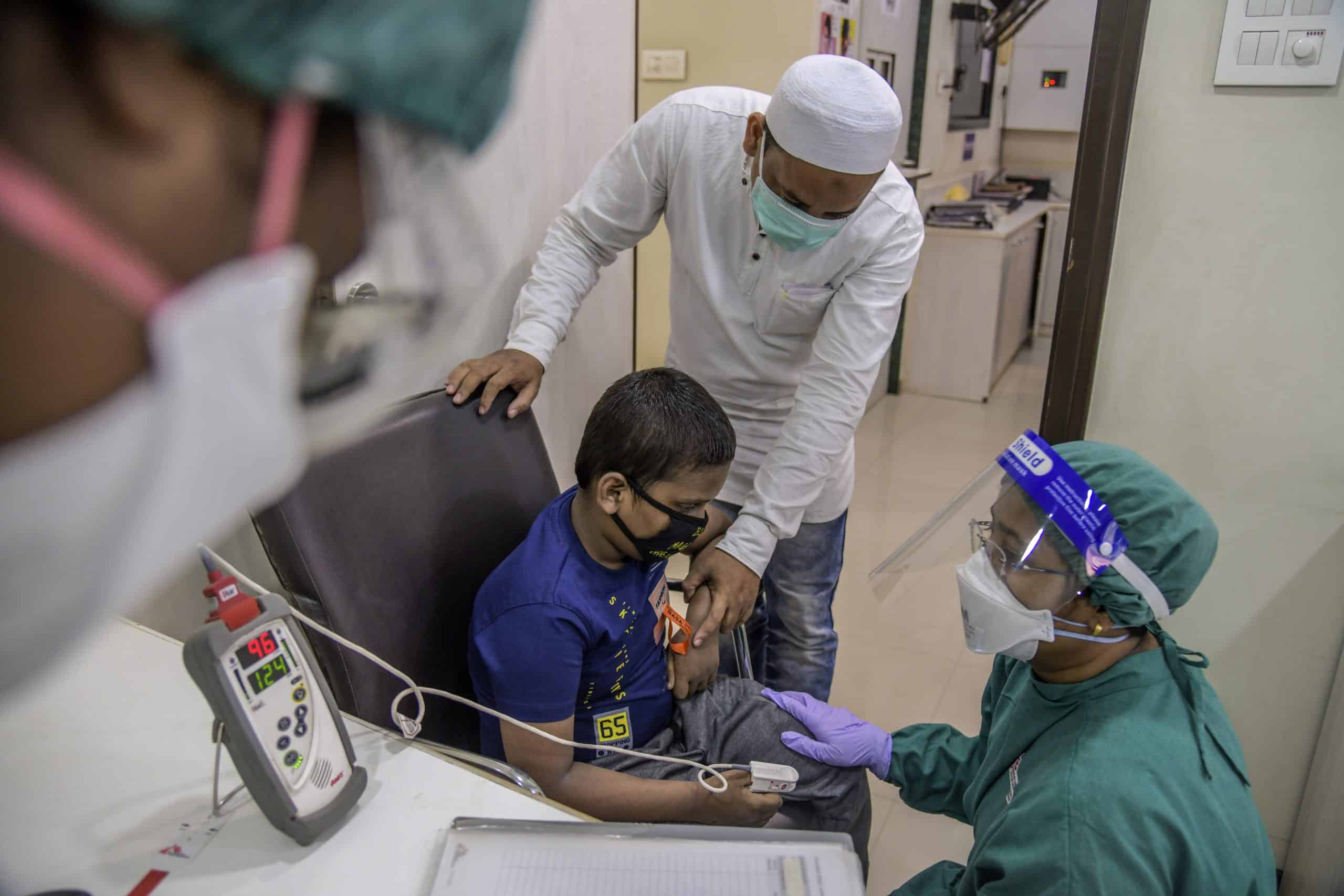
Infection control and mental health care
Patients who are on TB treatment are familiar with infection prevention controls (IPC) like wearing masks. But still, when people come to our clinic we put efforts to educate them about COVID-19 and ensure IPC measures are followed with mask-wearing and social distancing. We screen and triage patients for COVID-19 symptoms ensuring cases are identified early on.
During the first wave of COVID-19, there was much more panic and we saw a lot of fear among the patients. Now, there are extensive awareness programmes and people are allowed to isolate themselves at home if they test positive for COVID-19.
Our patient support team is reaching out to our patients over the phone to help them manage their anxiety and worries themselves while they’re isolating. If they need oxygen support they are referred to the hospital.
In our catchment area, there is a designated municipal health facility for the isolation of patients co-infected with TB and COVID-19 and for the management of mild and moderate cases. For any severe case management, patients are referred to tertiary care centres.
However, the number of critical care isolation bed available for TB patients with COVID-19 coinfection is very less. There is a need to have more such beds available on a wider scale especially for a densely populated city like Mumbai where the TB & DR-TB burden is high.
With an increasing load of COVID-19 cases in general, the system is quite overwhelmed, as many health facilities are being converted to COVID-19 care centres. This has made easy access to address other co-morbidities a challenge for the patients.
For patients with lung complications from tuberculosis, there are concerns that they may deteriorate faster. We’re also worried that people may not be accessing TB care because they are scared and worried about what will happen if they get COVID-19 and become severely ill.
Access to care for the migrant population
M-East ward is a high TB burden ward with more than 70% population living in slums. Many of the patients we treat are migrants who come to Mumbai looking for work and then settle down in the slums in M-East ward. They are daily wage workers and last year, during the first wave, they were particularly hit very hard. Many lost their jobs and were forced to return to their homes. For people with drug-resistant TB, this meant an interruption to their critical treatment as the drugs they required are often not available in smaller cities or rural areas. Our patient-support team worked hard to ensure continued care for these patients by linking them to the respective TB treatment centres in their native places with the help of the District TB officer and team. However, we were unable to reach many patients due to various issues.
In order to avoid the same situation this year, we’re proactively reaching out to our patients who are migrants asking them to contact us if they have to leave to their native places, so we can send a supply of medications to their local health centres and get in touch with their local medical teams. We need to ensure a smooth transition and continuity of care for them as they travel home. We’re also offering telephone counselling to help them with other problems they may face including the loss of work or difficulties obtaining their daily ration support. Our teams are offering psychological support and trying to find ways to collaborate with other organisations.

Vulnerable groups at risk
My biggest concerns are the knock-on effects of COVID-19 on other aspects of healthcare. Right now, many hospitals, health care centres and health care workers are being diverted to the COVID-19 response that other vulnerable patients living with TB, HIV, diabetes, hypertension or other chronic diseases are required to travel long distances to access medical care. Currently, it’s much harder for them to get the help they need. For example, TB patients would need proper isolation facilities for treatment to ensure infection control.
I am concerned about the oxygen availability and isolation bed capacity, including critical care, for patients co-infected with DR-TB and COVID-19. What will happen if patients start falling sick when we need a greater capacity for accommodating those with critical needs? If patients are waiting for surgery and they are being deprioritised because COVID-19 has to be dealt with first, then patients waiting for surgery may develop a lot more complications.
-
Related:
- coronavirus
- COVID-19
- India
- Mumbai
- Pandemic
- Tuberculosis











