Increasingly drug-resistant strains of tuberculosis (TB) are on the rise in India, particularly in hotspots such as Mumbai. Two new TB drugs, bedaquiline and delaminid, show promising results and offer renewed hope to patients whose TB strains are resistant to nearly all drugs available. But access to these new life-saving drugs in India remains greatly restricted, even for those most in need.

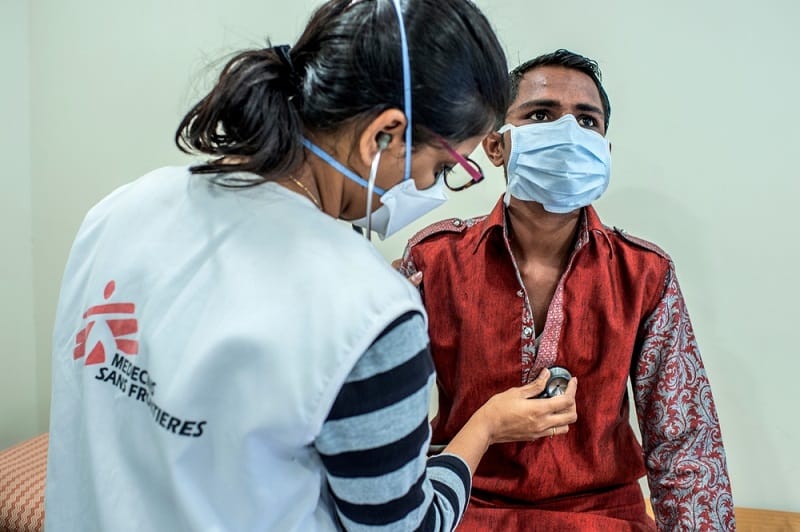
Hanif is 25 years old, lives in Mumbai, and is one of only a handful of extensively drug-resistant TB (XDR-TB) patients lucky enough to be able to have access to the new drugs. After having failed treatment for the fourth time, Hanif was referred to the clinic of Doctors Without Borders/Médecins Sans Frontiéres (MSF), an international medical humanitarian organisation who since 2006 provides free diagnosis, treatment and support to patients with drug-resistant TB in Mumbai.

After eight months of treatment using a combination of delamanid and bedaquiline together with other drugs, Hanif’s medical examinations show promising results and he is looking forward to getting back to normal life once again. However, he will need to continue taking his TB medication for twenty months more until he is fully cured.

Delamanid is currently only available in India through so-called compassionate use, where a special application for importing the drug needs to be made for each patient. This is a long process that can result in substantial delays in putting patients on treatment, which in turn could adversely affect their chances of survival. Apart from a government pilot program in six sites in India, Bedaquiline access is also restricted to just compassionate use.

Hanif lives with his wife, mother and two children in a small ground floor apartment, tucked away in an alleyway in the Govandi area of Mumbai. Like half of Mumbai’s population, he lives in an overcrowded slum where TB bacteria is easily transmitted due to the high population density and poor housing and environmental conditions. MSF has installed fans and ventilation shafts in the walls of Hanif’s house in order to improve airflow and to reduce the risk of family members getting infected.

Hanif used to work as a salesman in a shopping mall shoe shop, but had to give up his job when his health deteriorated.
“Initially I was OK and was on treatment, energetic, and had a normal weight, and could lift heavy things,” says Hanif. “But then suddenly my mind became blocked, I stopped interacting with people, I used to talk senseless blah-blah-blah and would trouble everyone a lot. I used to feel like a living corpse. Now I am feeling better, and am able to work. I am very happy because I’ve got a new life.”

Since the last five months, Hanif’s sputum samples show no traces of TB bacillus, which indicates that the medicines are working well. He is also much less likely to infect other people and does not need to wear a mask anymore. However, MSF’s stringent infection control protocols require all people to wear a mask while they are visiting the clinic.
Before being enrolled at MSF’s clinic, Hanif was receiving treatment on and off over a period of four years, from three different clinics. Patients seen by MSF have often previously been treated with ineffective regimens for several years by public and private practitioners. Some are also believed to have been directly infected in the community by extensively resistant strains.
“One of the clinics that provided me with drugs was a charity dependent on donations, and they sometimes would run out of money, ” says Hanif. “I missed some of the dosages as a result. I was bed-ridden and was coughing constantly. I couldn’t eat properly and couldn’t sleep at night. At that time, I felt that I was going to die.”

“The MSF doctors told me they needed to give me new drugs. I was told that these new drugs will work on me like new soldiers, which the TB germs are unfamiliar with. These new drugs took some time to come. I was eagerly waiting for them. For some three months, there was no news about the drugs. I had low appetite, started getting the fever in the evening, the cough increased and I experienced chills as well. Within days of getting the new drugs, my food intake increased, I started feeling better, and my cough stopped. I used to feel breathless even after walking twenty steps, but that disappeared slowly.”

Pooja Iyer is a counsellor with MSF and provides psychosocial support to patients who are suffering from drug side effects, stigma and depression. She also focuses on finding practical solutions to everyday barriers that patients may face in taking their treatment. Pooja has been counselling Hanif since he arrived a year ago, and says she is glad that his health is improving.
“When Hanif first came to us, he had fever chills and was extremely weak, and his mood was very low” she explains. “His mother would have to help him get to the clinic with the local train. When I see him now, there is a major difference. He’s glad that he’s gotten a job, he’s getting back on the track that he lost three years ago. He’s very motivated. It’s rewarding to see people come out of their illness, be happy, getting back to their job, getting out of stigma. I can really understand the pain they have to go through. The hardest part is to accept that there will also be a few deaths every now and then.”
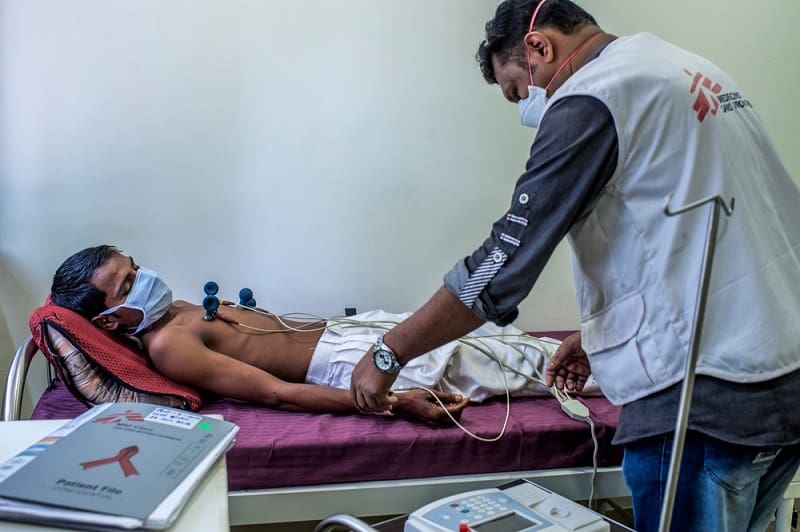
Through its project in Mumbai, MSF wants to demonstrate the importance of adequate TB testing, treatment and counselling, with a specific focus on the most resistant TB strains. All patients are fully tested to determine exactly which drugs they are resistant to. MSF then offers an individualised treatment regimen based on the resistance pattern. Counselling and psychosocial support are also offered in order to make sure that patients take their treatment correctly until they are cured.
“These drugs are really the last lifeline for many patients,” says Pramila Singh, MSF Clinic Manager. “We also have had patients who died before they could be put on treatment. Maybe they would have been alive today if the drugs had been available more easily. That’s why MSF advocates for the expanded roll out of bedaquiline and delaminid. Of course, with that, there also needs to be necessary safeguards to ensure professional management of these life-saving drugs.”

MSF in partnership with a local NGO facilitates vocational courses for recovering patients who are looking to return to working life after a long period of debilitating illness. But Hanif has already been offered a job once again as a shoe salesman in a shop. His manager has put him on a probationary period to see if he is fit enough to work. Every day, he travels for an hour on a train across town to reach the shop, located in a busy shopping area in downtown Mumbai.
“I think now I have the ability to work. In the long run, I would like to have my small business. This job is a kind of test for me, as I have come out of bed after so many months. Life has given me a second chance. My family has seen bad days, it is my responsibility to not to trouble them anymore and do something good.”

“There are many people with TB here in the community. I think it’s because of the living conditions, which are dirty and unhygienic. We have Mumbai’s dumping ground nearby. People living nearby to that smell it every day. The air is polluted and toxic. People sometimes don’t eat enough, and people spit on the road. Most of the time they are not aware that they have TB. They should go and get themselves tested. If they do this then there will not be any TB in Govandi. The government should also do check-ups of people in this area and put them on treatment.”

“Now I want to spend more time with my children. I think god has given me my kids as a gift. I want to take good care of them, and offer them a better life than what I have experienced.”
Photographs by Atul Loke/Panos Pictures











